Gestational Diabetes & The Mindful Birth: A Guide for CGMH, RVH, and HHCC Families
Reframing the Diagnosis: Your GD Journey
Receiving a Gestational Diabetes (GD) diagnosis can often feel like a shift in your birth "rhythm." Many families in the Georgian Bay and Dufferin County regions worry that this diagnosis automatically means a highly medicalized, restrictive birth experience.
As your Childbirth Educator and Doula, I am here to help you bridge the gap between clinical management and your mindful birth vision. A GD diagnosis is simply a data point—it does not define your capability to have a soulful, empowered, and even low-intervention birth at Collingwood General (CGMH), Royal Victoria (RVH), or Headwaters (HHCC).
The GD Screening: Understanding Your Options
In Ontario, the standard screening happens between 24 and 28 weeks. While the "orange drink" (Glucola) is the standard at labs like LifeLabs or Dynacare, you have evidence-based alternatives to discuss with your team:
The Fresh Test: A popular organic, non-GMO alternative made with crystallized lemon and mint. It meets diagnostic criteria but avoids artificial dyes like BVO or Yellow #6.
Home Monitoring: Some providers allow for 7–10 days of home blood sugar monitoring (testing 4 times a day) as an alternative to the glucose drink if you have sensitivities or severe nausea.
A1C Testing: While less sensitive for GD specifically, a baseline A1C can provide early data on how your body processes fuel.
Your Team: Providers & Protocols
Depending on who is catching your baby, your GD "rhythm" may look different. Here is how local groups in our area typically navigate a diagnosis:
Midwifery Care (Low-to-Moderate Risk)
Groups:Midwives Nottawasaga (Barrie/Collingwood), Barrie Midwives, and Midwives of Headwater Hills (Orangeville).
The Protocol: Midwives are specialists in normal birth. If your GD is diet-controlled, you typically stay in primary midwifery care. They often offer more space to discuss The Fresh Test or home monitoring.
Obstetrical Care (Collaborative & Specialized)
CGMH (Collingwood): You may work with Drs. Yeates, Stark, O’Toole, or O’Brien. They are known for a community-focused approach and work closely with midwives to keep your birth as "normal" as possible.
RVH (Barrie): Doctors like Drs. Adare, Fefelova, or Kilani manage higher-risk GD cases. At RVH, we focus on utilizing wireless monitoring so you can remain mobile.
HHCC (Orangeville): The OB team here works alongside the Diabetes Education Centre. If insulin is required, they may suggest a "mindful induction" closer to 39 weeks.
Leah’s Doula Tip: Navigating the Differences
The biggest difference you’ll notice is in the recommendation for induction.
Midwives may suggest waiting for spontaneous labour until 40 or 41 weeks if blood sugars are perfectly stable.
OBs may suggest a "mindful induction" closer to 39 weeks if insulin is involved, to mitigate the risk of the placenta maturing early.
Regardless of your provider, my role is to help you ask the right questions during these consultations: "Is this a recommendation or a requirement?" and "What are the benefits or risks of waiting another few days?"
Mindful Birth Strategies with GD
Movement as Medicine: Drawing on my yoga background, we use specific pelvic opening movements. Staying active during labour helps regulate blood sugar naturally.
Auditory Anchors: Stress can cause blood sugar spikes. We use relaxing music and soundscapes to keep your cortisol levels low.
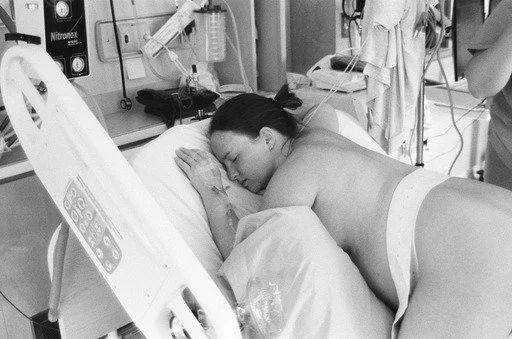
The Golden Hour: At HHCC and RVH, I prioritize protecting your skin-to-skin time. Early feeding is vital for stabilizing a GD baby’s blood sugar immediately after birth.
FAQs
Can I still have a "Natural Birth" with Gestational Diabetes?
1
Absolutely. Many people with GD have successful, unmedicated births. By focusing on prenatal education and staying active, you set the stage for a physiological labour.
Does GD mean I have to be induced at RVH or CGMH?
2
Not necessarily. While some providers recommend induction for GD (especially if insulin is used), many families successfully wait for spontaneous labour or choose a "Gentle Induction" method like a Foley Bulb.
How does GD affect my baby after birth?
3
The main concern is a temporary drop in the baby’s blood sugar (hypoglycemia). We prioritize immediate skin-to-skin and early breastfeeding (or colostrum expression) to naturally stabilize the baby’s levels.
Is The Fresh Test accepted at LifeLabs in Barrie or Collingwood?
4
Most providers at RVH and CGMH will accept The Fresh Test results, but you must confirm with your specific Midwife or OB first, as you usually need to provide the kit yourself.
How does a doula help with a GD induction at Headwaters?
5
If an induction is recommended at HHCC, I provide continuous support to help you "find your rhythm" when labour is facilitated. We use massage and aromatherapy to bridge the gap between medical intervention and mindful presence.
Can I still have a VBAC if I have Gestational Diabetes?
6
Yes. A diagnosis of GD does not disqualify you from a Trial of Labour After Caesarean (TOLAC). In fact, many studies show that for appropriately selected candidates, the success rate for a VBAC with GD remains high (around 64-70%).
The Mindful Edge: Because GD can sometimes lead to discussions about "big babies," we focus on optimal foetal positioning and pelvic mobility.
Our Strategy: At hospitals like RVH or CGMH, I help you navigate the extra monitoring required for both a VBAC and GD, ensuring you can still use your mindfulness anchors to stay calm and rhythmic.
What happens if my baby’s blood sugar is low after birth?
7
This is called neonatal hypoglycemia. The best "medicine" for this is immediate, uninterrupted skin-to-skin and colostrum.
Colostrum Harvesting: I encourage my GD clients to discuss "antenatal colostrum harvesting" (starting at 37 weeks) with their midwife or OB. Bringing small syringes of your own colostrum to Headwaters or RVH can be a game-changer, providing an immediate sugar boost for the baby without needing formula supplementation.
Will I still have diabetes after the baby is born?
7
For the vast majority of people, Gestational Diabetes disappears the moment the placenta is delivered. However, you will be asked to complete a follow-up Glucose Tolerance Test (the "orange drink" again, or an alternative) between 6 weeks and 6 months postpartum to ensure your levels have returned to baseline.
Postpartum Wellness: During our Gentle Ebb postpartum visits in Stayner or Barrie, we discuss how to maintain a balanced rhythm of nourishment to support your long-term health.
Book Your Mindful GD Birth Consultation
A diagnosis of Gestational Diabetes doesn't mean you lose your seat at the table of your own birth. Whether you are in Collingwood, Barrie, or Orangeville, I am here to ensure you have the evidence, the advocacy, and the mindfulness tools to birth with confidence.
Contact me today to book your complimentary 30-minute video or phone doula consultation.